CSAT and NPS Tracking for Healthcare and Insurance Contact Centers Meeting Compliance While Measuring Satisfaction

CSAT and NPS? They're the go-to metrics when you need to figure out how patients actually feel about your service. But here's the thing - they measure completely different aspects of the customer relationship.
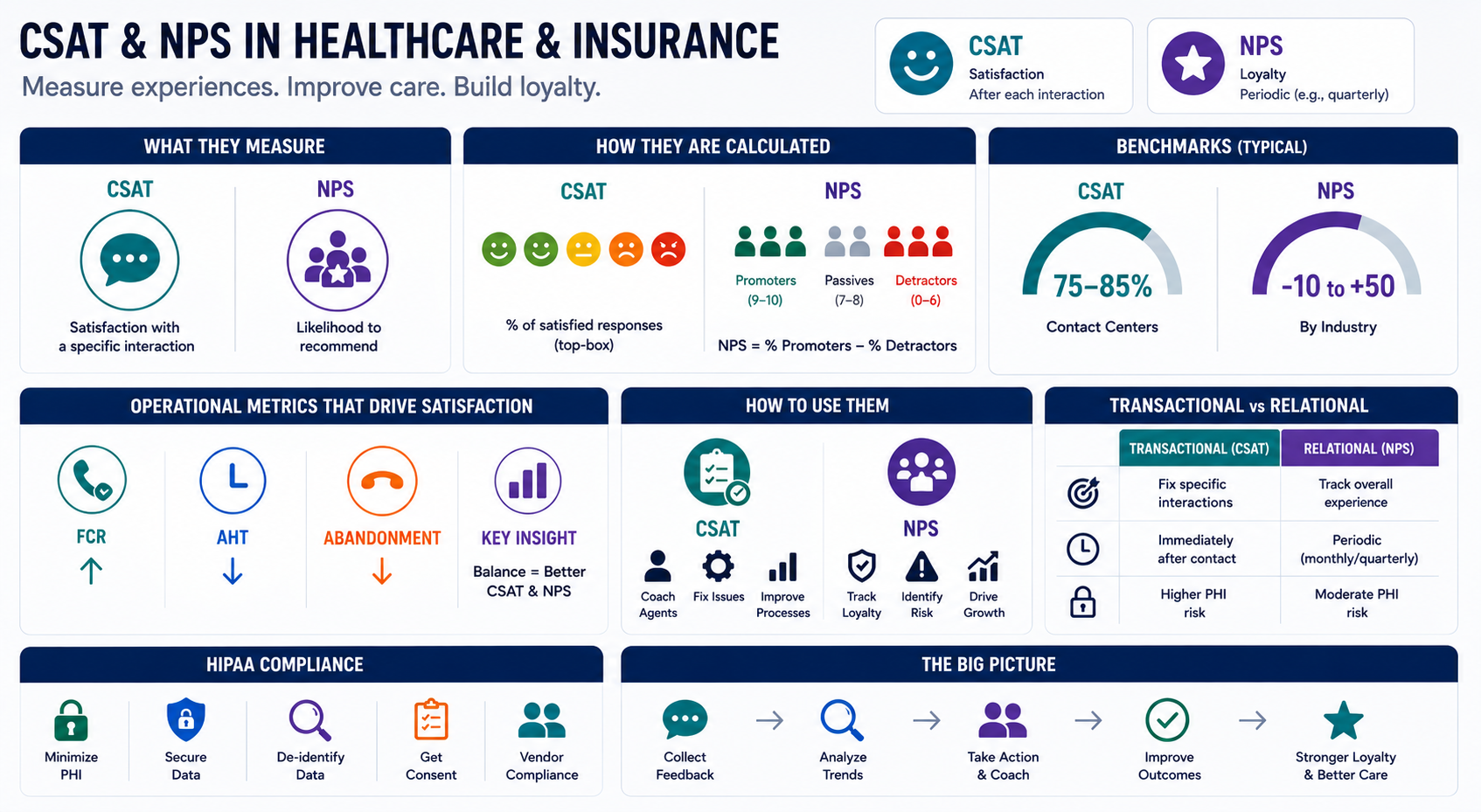
CSAT captures that immediate reaction right after a call or message. Think of it as the "how'd we do?" question at the moment of truth. NPS, on the other hand, takes a step back and asks about the bigger picture - would they actually recommend you to someone else? That's relationship-level stuff, and it reveals patterns over months, not minutes.
In regulated contact centers, the practical goal isn't rocket science: turn every patient interaction into data you can actually use to make better decisions. No fluff, just actionable insights that help you understand where things go wrong (and right) across the entire customer journey.
CSAT (Customer Satisfaction Score) happens right after an interaction ends. You're catching people while the experience is still fresh in their minds, which makes CSAT perfect for spotting specific problems tied to individual agents, particular queues, or recurring topics.
NPS (Net Promoter Score) operates on a different timeline entirely. It measures loyalty by asking that famous question - how likely are you to recommend us? - and you typically run it quarterly or annually because you're tracking long-term relationship health, not individual moments.
Here's what's interesting though. Healthcare organizations are starting to realize that traditional surveys miss huge chunks of their customer base. Surveys often measure what people remember about an experience rather than what actually happened in the moment. So yeah, use survey data, but don't treat it like it's the complete picture of your patient experience.
MetricWhat it measuresHow it's calculatedHow to use it------------CSATSatisfaction with a specific interactionPercent of satisfied responses (commonly top-box ratings)QA, coaching opportunities, channel and queue fixesNPSLoyalty and advocacy% Promoters minus % DetractorsRetention risk, account health, executive reporting
Let's talk benchmarks for a second. Contact center CSAT scores usually fall somewhere between 75 and 85%. NPS can swing from -10 to +50 depending on your industry.
For B2B healthcare and insurance brands, NPS often connects directly to account-level decisions and links to revenue retention and churn risk. Get this - 49% of companies using NPS also track at least one other metric, with CSAT being the most popular secondary choice at 33%.
One thing to remember: CSAT can jump around because of a single stressful episode, while NPS might lag behind what's actually happening in your operations right now.
The operational stuff explains the "why" behind patient satisfaction. These metrics help you make decisions based on evidence rather than guesswork about staffing, workflows, and coaching priorities.
First Call Resolution (FCR) usually improves patient satisfaction because nobody wants to call back three times for the same issue. Track FCR by issue type and you'll start seeing patterns in where your handoffs break down.
Average Handle Time (AHT) cuts both ways. Lower AHT might mean you're running an efficient operation, but if you're pushing agents to rush through complex healthcare and insurance conversations, you're probably sacrificing empathy and clarity. Not great for satisfaction scores.
Abandonment Rate tells you about the people who never even get to talk to an agent. Rising abandonment often signals access problems - long holds, poor routing, that kind of thing. Even if your CSAT surveys look strong, high abandonment might mean there's a whole group of silently dissatisfied people you're not hearing from.
Here's a practical tip: look at FCR and AHT together. When FCR drops while AHT falls, speed might be winning over accuracy, and satisfaction scores usually follow that trend downward.
Beyond these basic definitions, let's dig into how you actually implement these metrics while staying on the right side of industry regulations.
You can absolutely collect CSAT and NPS data in healthcare contact centers without breaking HIPAA rules. But only if you treat Protected Health Information like the compliance risk it actually is, not just during clinical workflows but throughout your entire satisfaction survey process.

HIPAA requires secure handling of PHI during satisfaction surveys and sentiment analysis (U.S. Department of Health and Human Services regulatory requirement). Your mission is building a continuous feedback loop that generates useful data for decision-making while keeping PHI exposure to an absolute minimum.
CSAT measures post-interaction satisfaction. Simple enough. But here's what matters - your team needs to define what "satisfied" actually means before you start reporting numbers. Is it top-box only? Top-two-box? Decide now, document it, stick with it.
NPS measures loyalty through that likelihood-to-recommend question. The math is straightforward: percent of "promoters" minus percent of "detractors."
Now, transactional versus relational feedback - they serve different purposes and carry different data risks:
Feedback typeBest used forTypical timingPHI risk profile------------TransactionalFixing service gaps in specific patient interactions, coaching, agent productivityImmediately after a call, chat, or claim updateHigher, comments often include identifiersRelationalTracking trust across customer journeys and overall patient experienceMonthly, quarterly, or program-basedModerate, still requires controls
Benchmarks vary wildly by organization, channel mix, and case complexity. Treat "NPS benchmarks healthcare insurance" as rough directional guidance, not gospel. Start with internal baselines by queue, reason code, and line of business before you worry about external comparisons.
HIPAA compliance requirements for patient data collection require secure handling of PHI during satisfaction surveys and sentiment analysis (HHS). You need HIPAA controls across intake, transmission, access, and retention - especially when you're collecting free-text patient feedback.
The biggest risks? Accidental PHI capture in transcripts, too many people having access to sensitive data, and sending PHI to tools that aren't set up to handle it properly. Here's a practical constraint worth remembering: free-text fields create the highest PHI leakage risk, so either limit them heavily or route them through controlled review processes.
Healthcare organizations must ensure survey platforms and data storage systems are HIPAA-compliant when collecting patient satisfaction metrics (HHS Office for Civil Rights guidance). That means getting a Business Associate Agreement (BAA) signed with any vendor handling PHI for surveys, storage, transcription, or analytics. Reference the HHS Office for Civil Rights HIPAA Privacy Rule when you're aligning internal policy with vendor workflows.
HIPAA-ready satisfaction data checklist
With compliance sorted out, we can focus on building a robust Voice of Customer program that actually listens to what patients are telling you.
A Voice of the Customer program in healthcare and insurance contact centers is basically a structured system for collecting, analyzing, and acting on patient and member feedback across every touchpoint. The goal isn't collecting more data - it's making decisions based on evidence that reduce service gaps, improve patient communication, and protect long-term trust.
VoC feedback should reflect the complete customer journey, not just a single survey score. In practice, that means capturing signals from multiple channels and connecting them to outcomes that leaders actually care about: agent productivity, smoother customer journeys, and fewer repeated contacts that delay care or claims resolution.
Using multiple metrics across channels gives you comprehensive insight into the experience ecosystem. Mapping all customer touchpoints and applying CSAT, CES, and NPS across channels provides that complete picture.
Build your collection methods around places where customers are already talking:
Timing matters more than you might think. CSAT should trigger within 24 hours of specific interactions like support calls, service delivery, or other post-interaction touchpoints.
To efficiently process all that feedback you're gathering, you'll need some serious analytical firepower. That's where AI-powered sentiment analysis becomes essential.
Sentiment analysis and AI help regulated contact centers understand emotion and intent at scale, using the actual language patients and members use rather than relying solely on post-call survey scores. In a healthcare contact center VoC program, that means you can identify frustration drivers in patient communication and fix service gaps faster while still controlling how Protected Health Information flows through your analytics.

Sentiment analysis classifies customer interactions into emotional signals - frustration, confusion, relief, whatever - using speech and language patterns.
Voice data: Speech analytics converts audio into time-stamped text, then models score sentiment by turn, topic, or specific moments in the customer journey.
Digital text data: Chat, email, and SMS can be analyzed directly with text mining to extract themes, sentiment, and recurring phrases that correlate with escalations or repeat contacts.
Use conversational intelligence to shift from asking "what's the score?" to "what caused the score?" and figuring out which team members can actually do something about it.
Identify specific drivers like benefit confusion, appointment access friction, or claims status uncertainty, then tie those patterns to coaching opportunities and agent productivity improvements. Build a continuous feedback loop that supports evidence-based decisions, including which knowledge articles aren't working, where transfers spike, and which scripts actually reduce patient interaction effort.
Contact Center Pipeline reports that conversational intelligence and AI tools provide richer insights beyond traditional surveys and help healthcare organizations directly address concerns that surveys can't capture. The same report notes growing demand driven by AI-powered support, shrinking chatbot development costs, and expanded omnichannel deployment.
Trade-off to plan for: sentiment models can completely misread sarcasm or stress, so keep human review for high-risk interactions and compliance-sensitive topics.
Even with advanced tools in place, certain challenges and pitfalls can derail your satisfaction tracking efforts.
CSAT and NPS programs fail when teams treat scores as the end goal instead of signals for action. CSAT and NPS metrics by themselves provide only a surface-level glimpse into customer-associate relationships, reflecting feelings about individual interactions rather than overall brand perception. The fix? Pair metrics with emotion-aware questions, conversation intelligence, and a closed-loop operating rhythm.
Strong insurance claims call center CSAT can still hide service gaps if your surveys don't capture what actually happened in the customer journey. Add a small set of "reason codes" tied to specific patient communication moments, then route themes to the team that can actually resolve them.
Owner hint: QA and Operations should define reason codes together, not just CX.
Metrics need action, technology, and deep questions that consider emotions behind customer service to produce meaningful insights. Use low-score interactions to target agent coaching and process improvement, balancing compliance constraints with practical scripts that improve patient satisfaction and patient experience.
Industry benchmarks vary by sector, interaction type, and methodology, so establish internal baselines and track improvement over time. This supports better decision-making, improves patient retention and loyalty, and enhances operational efficiency by reducing repeat contacts and unnecessary handling time.
Let's address the most common questions about CSAT and NPS tracking in this specialized environment.
HIPAA compliant sentiment analysis is required whenever a sentiment analysis tool or conversation intelligence platform processes patient interaction data that includes Protected Health Information. For regulated industry contact center satisfaction tracking, compliance isn't a side task - it's the operating constraint that determines what you can collect, where you can store it, and who gets access.
Key compliance baseline: patient satisfaction data collection must follow the HIPAA Privacy Rule (45 CFR §164.500) and HIPAA Security Rule (45 CFR §164.300) requirements (U.S. Department of Health and Human Services). In practice, healthcare organizations must ensure all sentiment analysis tools and conversational intelligence platforms are HIPAA-compliant when processing patient interactions (HHS Office for Civil Rights).
Evidence: See HHS Office for Civil Rights HIPAA Privacy Rule for regulatory requirements tied to 45 CFR §164.500.
A practical way to answer this question is focusing on four recurring failure modes that create preventable risk in healthcare contact centers:
Trade-off worth noting: aggressive analytics improves agent productivity and health outcomes only when controls prevent accidental exposure.
Next, we'll translate these compliance principles into insurance-specific metrics, constraints, and practical benchmarks.
Insurance contact centers often get too focused on post-call CSAT and miss the bigger churn signal. For B2B insurance brands, NPS should be your primary metric because it measures account-level loyalty and connects directly to retention and churn risk.
Use a three-metric approach that maps to how policyholders and brokers actually evaluate service:
Workflow hint: assign score ownership to Contact Center Ops, but route root-cause actions to Claims Ops and Underwriting, not just QA.
Benchmarks vary by line of business, but reported ranges are 75-85% for insurance contact center CSAT and -10 to +50 for NPS, depending on sector and service type (Source: Capacity, 2026). Treat insurance call center NPS compliance as a data-handling requirement: the safest programs separate survey analytics from sensitive identifiers, especially when running a patient experience analytics call center model across regulated interactions.
Now let's answer the most common questions teams ask about CSAT, NPS, and compliant sentiment analysis.
CSAT and NPS answer different business questions in healthcare and insurance contact centers. Use CSAT to fix specific breakdowns in patient communication and process steps, use NPS to guide long-term loyalty across customer journeys (Source: CallerDesk, 2025). The fastest path to value is turning survey scores and conversation intelligence into a continuous feedback loop that drives evidence-based decisions.
Q: What is NPS in call center? A: Net Promoter Score (NPS) is a loyalty metric that asks how likely a customer or patient is to recommend your organization. In regulated industry contact center satisfaction programs, NPS works best when you need a stable signal of relationship health across multiple interactions, not just one patient interaction (Source: CallerDesk, 2025).
Q: When should a healthcare or insurance team use CSAT instead of NPS? A: Use Customer Satisfaction (CSAT) when your goal is immediate action on a specific experience, like a claims status call, provider lookup, or benefits explanation. CSAT works as a tactical tool, while NPS guides long-term strategies and overall loyalty assessment (Source: CallerDesk, 2025).
Q: What is a good NPS for a call center? A: A "good" NPS depends on who's calling, why they're calling, and how your survey runs. For meaningful comparisons, benchmark against organizations with similar demographics, interaction types, and survey methodologies (Source: Capacity, 2026).
Q: What is a good NPS score for insurance industry? A: Treat NPS benchmarks healthcare insurance as directional guidance, not absolute targets, unless your comparison set is truly like-for-like. Otherwise, use internal trends by journey stage and channel to find service gaps that affect trust and renewal intent (Source: Capacity, 2026).
Q: How to improve NPS in a call center? A: Start by improving the drivers you can actually control: coaching and journey fixes. CSAT helps managers track agent performance, identify high-impact training opportunities, and measure improvements in specific processes.
Workflow hint: Assign clear ownership. QA owns root-cause tagging, Ops owns process fixes, and team leads own coaching to protect agent productivity.
Q: Can I use ChatGPT for sentiment analysis? A: Many teams use AI-driven sentiment analysis, but compliance comes first in healthcare and insurance call centers. Only analyze data in approved environments designed for HIPAA compliant sentiment analysis and insurance call center NPS compliance, and avoid submitting sensitive patient feedback into unapproved tools.
Bonus: Should you track CES too? A: Customer Effort Score (CES) is often worth adding because CES strongly predicts customer loyalty and future spending in healthcare and insurance contexts (Source: Balto AI, 2025).
To wrap up, here are the essential takeaways for successfully implementing satisfaction tracking.
In healthcare contact centers, patient satisfaction metrics should combine CSAT, NPS, and CES to connect patient satisfaction and patient experience from each interaction to loyalty (Balto AI, 2025).
Run regulated industry contact center satisfaction with insurance call center NPS compliance and HIPAA compliant sentiment analysis as constraints. Collect CES and insurance claims call center CSAT after support interactions for coaching and agent productivity, run quarterly NPS, and compare shifts to validate NPS benchmarks healthcare insurance (Balto AI, 2025).
A voice of customer healthcare contact center program should add patient experience analytics call center reviews and AI-driven sentiment analysis to surface service gaps surveys miss (Contact Center Pipeline, January 2025). Route patient feedback to owners for data-driven business decisions that improve health outcomes, raise operational efficiency, and reduce costs.